
1) How should we behave with food during vacation time?
There shouldn’t really be a difference between winter and summer when it comes to healthy eating habits.
That said, the arrival of summer and vacations can be a great motivation to start taking care of your diet and health.
Begin by following a balanced and personalized diet that suits your body and lifestyle.
2) Which foods should we prefer, and which should we avoid?
Focus on:
- Seasonal fruit and vegetables
- Whole grains
- Fish
- Lean meats
Avoid over-processed, overly fatty, or sugary foods. Balance and variety are key.
3) Can I enjoy an aperitivo while on vacation?
Absolutely, but in moderation.
Wine and prosecco are among the lower-calorie alcoholic beverages.
An occasional glass can replace a snack, but avoid pairing it with too many high-calorie appetizers.
4) What are some light, complete meal options for summer?
Choose meals with a good balance of carbohydrates, fats, and proteins, such as:
- Couscous with tomatoes, arugula, and tuna
- Black rice with zucchini and shrimp
- Mixed salad with grilled chicken or turkey and a slice of whole grain bread
5) How should we incorporate fruit into our summer diet?
Fruit is essential and should be eaten regularly:
- As a morning or afternoon snack
- At breakfast
- Or after meals
It helps keep you hydrated and nourished.
6) Hydration: how, how much, and when should we drink?
Aim to drink at least 2 liters of water per day, and even more depending on:
- Outdoor temperature
- Physical activity
- Personal needs
If you struggle with plain water, try infusing it with lemon, mint, or ginger.
7) Sun and tanning: how can we protect ourselves through diet?
Support your skin with foods rich in:
- Carotenoids (carrots, pumpkin, bell peppers, dark leafy greens)
- Vitamin C (berries, citrus fruits, kiwi, tomatoes)
- Omega-3 fatty acids (oily fish like salmon, and nuts)
- Vitamin B (whole grains like rice, millet, farro)
8) Do I have to give up ice cream in the summer?
No!
You don’t have to give up anything completely.
An artisanal or fruit-based ice cream can be enjoyed every now and then, perhaps in place of a snack.
9) Summer and carb phobia: how to handle it?
The fear of carbohydrates is unfounded and not seasonal.
Carbs provide energy, so they should always be part of your diet—just choose the right kinds and portions.
10) Final advice for a better summer?
- Maintain a healthy, balanced lifestyle
- Eat a variety of seasonal foods in the right portions
- Stay hydrated
- Be active—even if it’s just beach games or hiking
That way, you can enjoy a gelato, an aperitivo, or a dinner out without guilt.
What is Labiaplasty?

Labiaplasty is a surgical procedure to reshape the external female genitalia, aimed at restoring a natural appearance and size to the labia minora and/or labia majora.
When the labia minora are excessively large or have an irregular shape, a reduction procedure can be performed. This reductive labiaplasty is often combined with procedures that increase volume in the labia majora, using hyaluronic acid fillers or fat grafting (lipofilling).
It is typically a same-day outpatient procedure, meaning the patient can go home the same day and does not require hospitalization. The surgery usually lasts 60 to 90 minutes.
Why Is It Performed?
The most common reasons for undergoing labia reduction surgery include:
- Enlarged or elongated labia, which cause discomfort when wearing certain clothing
- Discomfort during activities such as cycling, walking, or sexual intercourse
- Changes in the shape or size of the labia after childbirth that cause physical or emotional discomfort
What Does the Procedure Involve?
The surgery involves the removal of excess tissue using the technique recommended by the surgeon (rim excision or wedge excision). The incisions are closed using absorbable stitches.
Labiaplasty can be performed under local or general anesthesia.
It is normal to experience mild discomfort and swelling for a few days after surgery. These symptoms usually improve after 3–4 weeks and can be managed with pain relief medication.
An ice pack can also help relieve discomfort and reduce swelling—but it should never touch the skin directly. The ice should be wrapped in a soft towel to protect the skin.
Recovery Timeline
- Return to work is usually possible after one week.
- Normal daily activities can be resumed after 2–3 weeks.
- Sexual activity, cycling, and horseback riding should be avoided for 4–6 weeks after surgery.
- Internal tampons should not be used during the first 6 weeks post-surgery.
Scars in this anatomical area typically heal quickly and are usually barely noticeable.
How to Prepare for Labiaplasty
- It is recommended to stop smoking at least 4 weeks before the surgery.
- Full hair removal of the genital area is necessary prior to the procedure.
Postoperative Care
In the days following the surgery, it is important to follow these guidelines:
- Wear comfortable, natural-fiber underwear, preferably undyed. Avoid thongs or G-strings for at least 6 weeks post-surgery.
- Do not drive for 1 week after the procedure; arrange for someone to escort you home on the day of surgery.
- Gently wash the area daily in the shower (do not use a direct water jet on the surgical area). Pat dry gently with a clean, soft towel.
- Rest for at least 24–48 hours post-op. Returning to work may vary per individual, but light daily activities can typically resume by the first week.
Bilingualism: Facts and Myths

What do we mean by bilingualism?
Bilingualism is the ability to understand and/or use two or more languages.
The term therefore also includes multilingualism, referring to the knowledge and/or use of several different languages.
A bilingual individual does not necessarily have equal fluency in both languages.
Moreover, bilingual people are able to use one language over another depending on the context and purpose—for example, in family settings or at school. Therefore, a bilingual person may not have the same communication skills in both languages.
Bilingualism is not a disorder, and there is no scientific evidence that it causes or contributes to any language or communication difficulties.
Language is fundamental to a person’s identity, reflecting the culture connected to it. It is therefore essential to respect and value the multilingual identity of individuals.
L1 and L2
When we talk about bilingualism or multilingualism, we refer to L1 and L2.
- L1: the primary language to which a person is exposed—often called the “mother tongue.”
- L2: a second language, typically acquired later, most commonly through school or structured environments.
Some bilingual individuals learn two languages simultaneously from birth. Even in these cases, a perfect balance between the two languages is rare.
Types of Bilingualism and the “Silent Phase”
There are two main types of bilingualism:
- Simultaneous bilingualism: when an individual is exposed to two or more languages from birth. This does not mean the exposure is equal across languages.
- Sequential bilingualism: when the second language (L2) is acquired after initial exposure to the first language (L1). This typically happens in school settings when children begin to hear and use a different language than the one spoken at home.
The “silent phase” can occur when a child enters a school environment where the language spoken is different from their mother tongue.
During this phase, the child realizes their first language cannot be used to communicate and begins acquiring L2. This is a natural stage in second-language acquisition.
Scientific literature suggests that if this phase lasts more than one month after L2 exposure, a consultation with a specialist may be advisable.
However, other studies indicate that the silent phase can last up to six months or even a year. It’s important to follow professional guidance to best support communication development during this time.
The Effects of Bilingualism on the Brain
Being exposed to more than one language is a tremendous asset. Many studies have investigated how bilingualism affects cognitive and neural systems—with impressive results.
Research has found a strong correlation between bilingualism and effective cognitive control.
In bilingual individuals, both languages are activated at once (language co-activation). The constant need to manage attention between two languages and to select the correct one for the context and interlocutor (code-switching) strengthens executive control mechanisms.
Bilingual speakers tend to show:
- Better ability to ignore irrelevant information
- Enhanced concentration
- Greater resistance to distraction
Neuroimaging techniques have also shown that learning and using more than one language throughout life stimulates areas of the brain involved in language processing and executive functions—resulting in increased volume and thickness in those regions.
Protection Against Cognitive Decline
When a second language is learned in adulthood, the brain’s ability to change (neuroplasticity) is more limited, meaning that learning may take more time and effort.
However, the benefits of bilingualism extend beyond childhood. A study by the University of York found that bilingualism enhances cognitive reserve, potentially delaying the onset of early Alzheimer’s symptoms.
These findings suggest that bilingualism may have a protective role against cognitive decline.
By Cecilia Brogi and Nicole Luciana Zocchi
Back Pain: Acute vs Chronic
Prevalence
Low back pain is the leading cause of disability in the UK, with estimates showing that 8 out of 10 adults will experience at least one episode during their lifetime. We spoke with our physiotherapist, Pietro Mazzariello, who shared key insights on this common issue.
“While most cases resolve within a few weeks,” says Pietro, “20% of people require medical support, and about one-third experience recurring episodes, which can lead to chronic pain.”
He adds: “30% of people who have had back pain before will experience another episode within 6 months, and about 40% within a year of the previous one.”
How Does It Manifest?
An episode of low back pain can come with a range of symptoms and severity, often causing fear and concern. In fact, 40% of people describe their pain as a burning or numb sensation radiating down the legs.
When struck by such sudden and intense pain, the first thought is often that something serious or damaging has occurred. Fortunately, only 1% of cases are due to serious conditions that may require surgical intervention.
Who to Turn To and How?
Your GP or physiotherapist is well-equipped to assess the underlying causes through a thorough clinical evaluation.
Diagnostic tests like X-rays or MRI scans are only necessary in specific cases.
“Studies show that MRI results are clinically relevant in only 5 out of 100 cases of low back pain,” says Pietro.
Risk Factors
As with many musculoskeletal conditions, it’s often not possible to pinpoint a single cause. Back pain is multifactorial, and effective management involves a holistic approach, addressing lifestyle-related elements such as:
- Nutrition
- Sleep quality
- Emotional and stress management
- Physical activity and exercise
There is strong evidence that chronic or persistent low back pain is linked to poor identification and management of these factors, and the adoption of unhelpful behaviors that follow.
In Conclusion
If your pain persists for more than a few weeks, consulting a physiotherapist can greatly help accelerate recovery, prevent chronic pain, and improve your quality of life.
By our physiotherapist Pietro Mazzariello
Physical Activity During Pregnancy

By our midwife Katia Ciccarella
Too often, expectant mothers still believe that pregnancy necessarily means limiting—or even stopping—physical activity. Unless prescribed for specific medical reasons, absolute rest during pregnancy can lead to excessive weight gain, reduced awareness of bodily changes, physical discomfort (such as back pain, swelling in the legs and ankles), and even emotional distress.
In this post, we aim to clarify current guidelines and debunk some common myths.
Benefits and Features of Physical Activity During Pregnancy
For low-risk pregnancies, international guidelines (RCOG, ACOG, SIGO, and Italy’s Istituto Superiore di Sanità) recommend at least 150 minutes of moderate physical activity per week—around 30 minutes a day, which can be divided into 10-minute sessions.
The benefits are numerous:
- Improved cardiorespiratory fitness, enhancing oxygen exchange between mother and baby
- Better weight management
- Reduced nausea and fatigue
- Enhanced muscle endurance, helpful during labor and postpartum recovery
- Prevention of back pain and other muscular discomforts
- Lower risk of preeclampsia, gestational diabetes, hypertension, and cesarean birth
- Decreased and prevented depressive symptoms
Contraindications
Pregnancy is not, by itself, a contraindication to exercise. However, it’s always best to consult with your obstetrician or gynecologist.
There are absolute and relative contraindications:
Absolute Contraindications (Exercise not advised):
- Significant heart disease
- Restrictive lung disease
- Incompetent cervix (with or without cerclage)
- High-risk multiple pregnancy
- Persistent vaginal bleeding in the second or third trimester
- Placenta previa after 26 weeks
- Preterm labor in current or past pregnancies
- Preeclampsia or pregnancy-induced hypertension
- Ruptured membranes
- Severe anemia
Relative Contraindications (Case-by-case):
- Mild anemia
- Mild cardiac arrhythmias
- Chronic bronchitis
- Poorly controlled type 1 diabetes, hypertension, epilepsy, hyperthyroidism
- Morbid obesity (BMI > 40)
- Severe underweight (BMI < 15)
- Extremely sedentary lifestyle
- Intrauterine growth restriction in current pregnancy
- Orthopedic limitations
- Heavy smoking
Which Activities Are Safe During Pregnancy?
Most sports and forms of exercise are suitable for pregnancy (across all trimesters), including:
- Running
- Cycling (especially indoor)
- Swimming
- Aerobics
- Strength training
- Yoga
- Pilates
However, keep in mind:
- The goal is to maintain overall fitness and health, not to improve performance. As pregnancy progresses, you may need to reduce intensity and movement range.
- It’s never too late to start. Even sedentary women are now encouraged to begin gradually, e.g., brisk walking.
Always seek guidance from qualified fitness professionals, ideally with pre/postnatal certifications, and make sure your midwife has approved your plan.
Importantly, moderate physical activity does not increase the risk of miscarriage in the first trimester. Fatigue is normal in early and late pregnancy—listen to your body, but don’t stop exercising completely, especially if you were active before.
Which Activities to Avoid?
Avoid high-risk and contact sports, including:
- Football, rugby, martial arts, basketball, boxing
- Horseback riding, climbing, artistic gymnastics, off-road cycling, skiing
- Scuba diving
- Skydiving
- High-altitude sports (above 2000 m)
- Hot yoga or hot pilates
After the first trimester:
- Any sport involving risk of abdominal impact (e.g., tennis, squash)
- Exercises lying on your back (supine position) after 16 weeks, especially if you experience dizziness or nausea in this position
When to Stop and See a Specialist?
Immediately consult your doctor or midwife if you experience:
- Vaginal bleeding
- Painful or regular contractions
- Leakage of amniotic fluid
- Shortness of breath after activity
- Chest pain
- Severe headaches unrelieved by paracetamol
- Muscle weakness affecting balance
- Sudden calf pain or swelling (unrelated to exercise)

By Dr. Elisa Gatti and Dr. Cristina Vismara
Two years after the onset of the pandemic, in a time when society is being encouraged—legislatively and culturally—to return to “normal,” it can be useful to reflect from a psychological and emotional perspective.
We started from a state of heightened alert and activation, marked by destabilizing emotions like fear and anguish. We were faced with a danger that was both unknown and deadly, as well as the hope and fantasy of finding a “cure” that would allow us to eliminate it and return to the life we once knew—one that felt safe.
Over time, however, we have been learning to coexist with COVID. We are gradually getting to know it and learning to manage it thanks to ongoing scientific progress. The initial emotional intensity is giving way to slower, more enduring feelings, and likely a growing awareness that this is not a 100-meter sprint, but a marathon. The finish line isn’t where we thought it was, and both body and mind need to reorganize to keep going.
So what kind of outlook can we have on the present and the future?
Can we allow ourselves to live with the pandemic—without being overwhelmed by anxiety or pretending it doesn’t exist? The variables to consider are certainly increasing, but complexity can be managed.
What is happening to us psychologically?
Like during a marathon, the body and mind slowly adapt to the demands of this new reality and the shift in habits. But this adjustment comes with emotional and relational effort.
Many psychological processes occur unconsciously. Reflecting on our inner emotional states can support and ease the journey.
From a psychological standpoint, we are dealing with the realization that things may never return to exactly how they were. This involves mourning the loss of that belief and reworking our expectations, life plans, and vision of the future. This must be acknowledged to process it psychologically and to allow ourselves to live in this new dimension.
Is it normal to feel more insecure?
Absolutely. The awareness that our current reality is constantly evolving amplifies a sense of unpredictability, which can fuel anxiety.
We’re forming a new perception of risk and safety, for ourselves and our loved ones, depending on our family structure and relational context.
These shifting perceptions, alongside mobility limitations and remote work, have impacted social relationships. Rebuilding our social network now requires more intentionality and energy. It involves renegotiating relationships in light of changed circumstances and perceptions of others.
The third runner in our marathon—COVID—that we hoped to leave behind after 100 meters, is still running beside us. Sometimes fast and aggressive, sometimes weak and slow, but always there—shaping how we relate to ourselves and others, and how safe we feel in those relationships.
So what can we do?
That’s a valid and understandable question. But when it comes to emotions, sometimes the answer is not about “doing” but about allowing ourselves to simply be—recognizing our inner resources to cope with what we’re feeling or acknowledging when we need help.
A good starting point is to maintain awareness of ourselves: observe our emotions, understand their context, and pay attention to the signals our body and relationships are sending.
Staying in touch with ourselves enables us to discover new, personal ways to adapt to the evolving world around us.
Which signs of distress should not be ignored?
It’s important to seek professional help when emotional discomfort starts to affect daily wellbeing, interferes with our ability to fulfill important roles (as parent, professional, child), or causes tension in close relationships (with partners, children, or colleagues).
Some concrete warning signs include:
- Persistent anxiety
- Panic attacks
- Mood swings or depressed mood that limits motivation for daily activities
- Sleep disturbances
- Disordered eating
- Irritability, anger outbursts
- Obsessive or ruminating thoughts
- Somatic symptoms without organic cause
Once these internal signs of distress are recognized, the next important step is to remember that asking for help is a strength. It can become an opportunity to reconnect with yourself, to understand your symptoms and signals more clearly, and to know that you are not alone on this journey.

Colorectal cancer is a type of cancer that forms in the tissues of the colon (the longest part of the large intestine) or the rectum (the portion of the intestine closest to the anus).
Like all cancers, colorectal cancer results from the uncontrolled growth of cells, in this case the epithelial cells of the mucosa lining the inside of the intestine.
Cancers of the intestine mainly originate in the colon and rectum, while cancers of the small intestine and anal canal are much rarer (2–3% of all digestive tract cancers).
Colon cancers are nearly three times more common than rectal cancers and may present with different symptoms.
Dr. Alex Leo provides an overview of colorectal cancer and the latest research advances in the field.
According to GLOBOCAN 2020 estimates from the International Agency for Research on Cancer (IARC), colorectal cancer accounts for 10% of all diagnosed cancers worldwide, ranking third in incidence after breast and lung cancers.
This disease is relatively rare before the age of 40 and occurs more frequently in individuals aged 60 to 75, with little difference between men and women.
Risk Factors
Known risk factors for colorectal cancer are related to diet, genetics, and other non-hereditary causes.
Most colorectal cancers develop from the malignant transformation of polyps, small growths caused by the proliferation of mucosal cells in the intestine.
However, not all polyps have the potential to become cancerous.
In general, polyps do not cause symptoms, though in some cases they may lead to minor bleeding, detectable through a fecal occult blood test.
In other cases, larger bleeding visible to the naked eye or even true rectal hemorrhages may occur.
Early symptoms—such as fatigue and loss of appetite—are often vague, sporadic, and may be overlooked by patients, especially younger ones.
More serious symptoms, including anemia and unexplained weight loss, can also be ignored.
Persistent constipation, alternating with diarrhea, or irregular bowel habits, may be early warning signs that should not be underestimated.
Diagnosis
Patients presenting these symptoms should consult a specialist gastrointestinal surgeon.
Diagnosis typically includes:
- a clinical history,
- a physical examination, and
- diagnostic tests.
A minimally invasive test, such as a sigmoidoscopy, may be sufficient in some cases.
What is a Sigmoidoscopy?
A sigmoidoscopy is a diagnostic procedure that allows doctors to examine the lower third of the colon.
It is useful for identifying the cause of abdominal pain, constipation, abnormal growths, or bleeding.
It can also be used to collect biopsies or to perform procedures like the removal of polyps or hemorrhoids.
A lighted tube, called a sigmoidoscope, is inserted through the anus, and air is insufflated into the colon for better visualization.
Sigmoidoscopy is typically performed on an outpatient basis and does not require anesthesia.
If necessary, the specialist may recommend a colonoscopy—a more invasive test performed by gastroenterologists in specialized centers. Colonoscopy is usually done under sedation, and rarely under general anesthesia.
Before the Procedure
- For an outpatient sigmoidoscopy, no preparation is needed.
- If a more invasive procedure is recommended, bowel preparation will be required.
How Long Does It Take?
An outpatient sigmoidoscopy usually lasts no more than 5 minutes.
Including the complete medical consultation, the entire appointment typically takes about 10 minutes.
Is It Painful?
Sigmoidoscopy is generally not painful. Some discomfort may be felt.
However, if the patient has acute conditions, such as anal fissures, the procedure may be painful—in these cases, it is not performed.

Having an efficient immune system is essential to protect us from illness and infection. This is always true, but especially so during a public health emergency like the one caused by COVID-19.
What can we do to improve our immune defenses?
The immune system’s activity is strongly influenced by our diet. To function properly, it requires an adequate intake of both macro- and micronutrients. Ensuring a varied and balanced diet is key to receiving all the essential compounds needed for optimal immune performance every day.
A healthy gut also plays a vital role in maintaining strong immune defenses. To support gut balance, it is important to consume at least 30g of fiber per day, sourced from legumes, vegetables, and fresh fruits (aim for five servings daily), as well as include probiotics in the diet—naturally found in yogurt and kefir.
Our Dietitian Ilaria Carandente’s Insights
Tell us about the role of micronutrients:
Certain vitamins and minerals are particularly important for the immune system’s effectiveness:
- Vitamin C: A powerful antioxidant with immune-boosting properties. Deficiency increases susceptibility to infections. Common sources include citrus fruits, but also bell peppers, tomatoes, kiwi, and leafy greens. This vitamin is sensitive to light, heat, and oxygen, which reduce its levels in food. To preserve it, eat or cook vitamin C-rich foods right after cutting them (like fresh orange juice, which should be consumed immediately). Avoid soaking vegetables for too long, as it is a water-soluble vitamin. Cooking methods also matter: boiling, steaming, and baking lead to significant losses, while vacuum cooking or pressure cooking preserve it better.
- Vitamin D: An immune modulator mainly produced by the skin when exposed to sunlight. Food is a lesser source and includes only a few animal-based products, such as salmon, sardines, herring, tuna, swordfish, eggs (especially the yolk), and cheese. The only plant-based sources with notable vitamin D content are some mushrooms—porcini, chanterelles, and honey mushrooms.
- Vitamin E: Has antioxidant properties and helps maintain immune cell health. It’s found in nuts (almonds, hazelnuts, peanuts), vegetable oils (olive, seed, sunflower), avocados, and leafy green vegetables.
- Zinc and selenium: Both have strong antioxidant effects. They are abundant in nuts (pistachios, almonds, cashews, walnuts), with smaller amounts in legumes and whole grains.
What about Omega-3s?
Omega-3 fatty acids are also powerful allies of the immune system, helping to regulate immune responses and inflammation. They are primarily found in fatty fish (especially sardines, mackerel, herring, but also salmon, tuna, and cod), nuts (particularly walnuts, hazelnuts, almonds), leafy greens, soy, and avocados.
Is there a recommended diet?
In general, the Mediterranean diet remains an excellent model to follow. It provides a balanced intake of all macro- and micronutrients needed for strong immune function and overall health.
Can we use vitamin supplements during winter?
Vitamin and mineral supplements may be necessary only in cases of restrictive diets, food intolerances or allergies, or medical conditions that require avoiding specific foods or food groups. Even then, supplementation should be personalized and preferably prescribed by a physician. It’s important to remember that no supplement can replace a fundamentally unbalanced diet.
Visual Snow Syndrome
Imagine seeing the world through a thick veil of static—like the “snow” on an old television with no signal.
Now imagine seeing this constantly, without relief, and not being able to explain to anyone exactly what you’re seeing.
This describes quite accurately the daily life of a typical patient with Visual Snow Syndrome (VSS).
What is Visual Snow?
Visual Snow is a neurological condition, only recently described, which manifests as a continuous visual disturbance. Patients see countless small, flickering dots—like visual “snow”—across their entire field of vision.
But the condition doesn’t stop there.
Many patients also experience:
- Palinopsia: lingering images even after the object is gone
- Photophobia: heightened sensitivity to light
- Nyctalopia: difficulty seeing at night or in dim light
- Entoptic phenomena: such as floaters, which are common even in healthy individuals, but become constant and intrusive in Visual Snow
Diagnosis Challenges
A typical Visual Snow patient may go years without a diagnosis.
Why?
- Because it’s a sensory disorder that’s hard to identify without listening closely to the patient’s description
- Because standard eye exams usually show no abnormalities
The problem doesn’t lie in the eyes, but rather in how the brain processes visual information.
How Common Is It?
Though it was long unrecognized, recent research suggests it’s not rare.
A study from the UK estimated that up to 2% of the population might have a form of the condition, ranging from mild disturbances to full-blown syndrome.
In more severe cases, VSS can be debilitating, especially when it includes all the symptoms described above and is associated with common comorbidities like:
- Migraine
- Tinnitus (ringing in the ears)
What Causes It?
The causes are still not fully understood.
However, brain imaging studies (from King’s College London) show dysfunction in the visual processing areas of the brain—especially the visual cortex.
We spoke with Dr. Francesca Puledda, a neurologist specialised in this condition and in headache disorders.
Can Visual Snow Be Treated?
Unfortunately, no specific treatment or medication currently exists for VSS.
Management must be individualized, focusing on the most disabling symptoms and often requiring an integrated, multidisciplinary approach.
Is Visual Snow Caused by Anxiety?
No.
Visual Snow is not caused by anxiety or psychological disorders.
However, these issues often co-occur, particularly because:
- A sudden onset of symptoms can lead to distress, anxiety, and depression
- The constant visual disturbance can impact quality of life
A timely diagnosis and psychological support can help manage the emotional burden—but it’s essential to distinguish the neurological origin of the condition from any psychiatric symptoms that may follow.
What Should I Do If I Think I Have Visual Snow?
If you have symptoms that started suddenly or are interfering with your daily life:
If needed, they will refer you to a neurologist who specializes in sensory processing disorders
See your primary care doctor
They may order an eye exam to rule out ocular problems
Rosacea: Does It Get Worse in Winter?
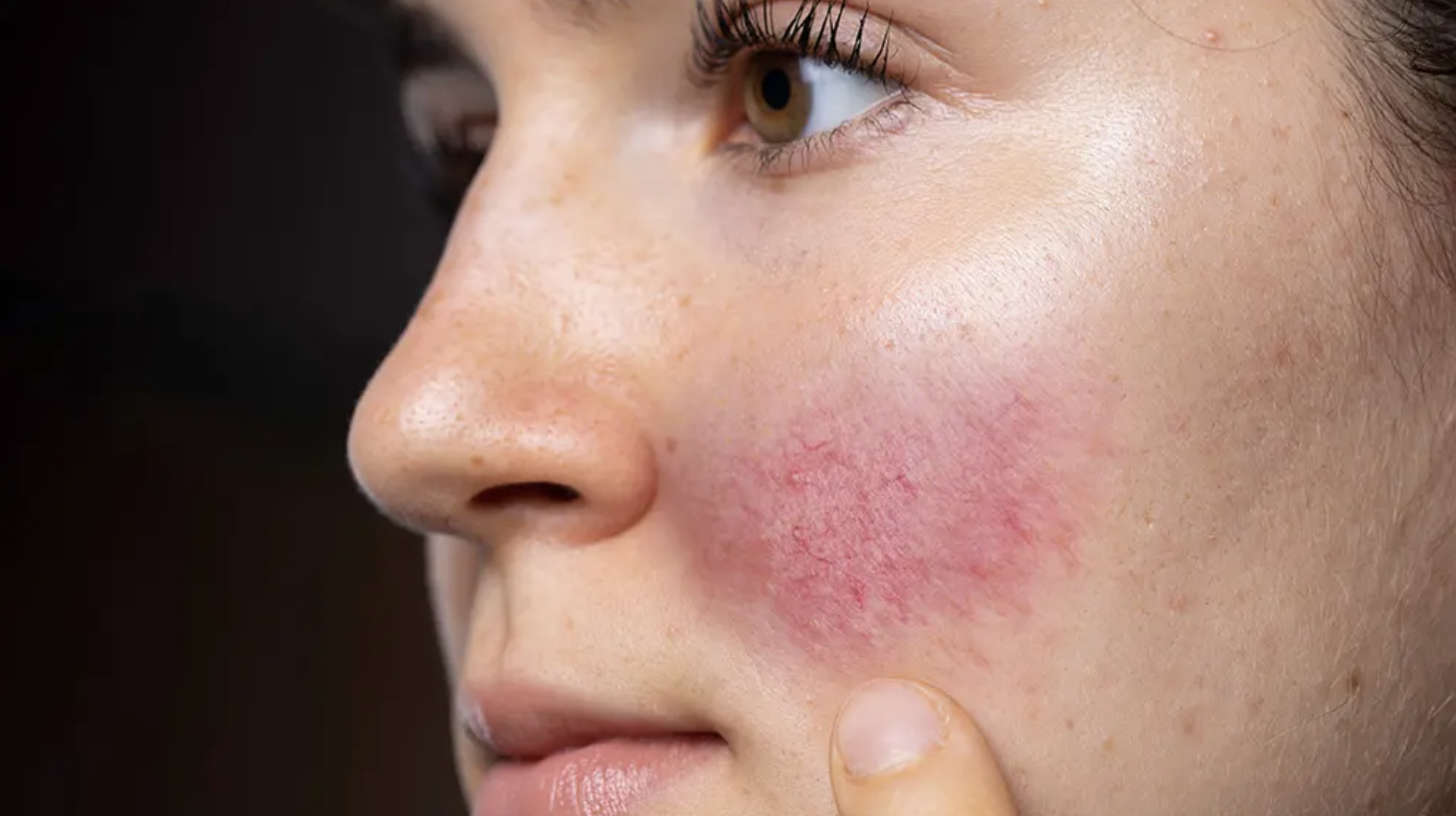
Rosacea is an inflammatory skin condition. Factors such as obesity, smoking, and excessive alcohol consumption can contribute to its development. The most common form—erythematotelangiectatic rosacea—is widely known as couperose. It’s essential to understand what should be avoided and what can be used in managing the condition.
We discussed this with Dr. Sara Pruneddu, our dermatologist.
What causes rosacea?
The exact causes of rosacea are still unknown, but several contributing factors have been identified:
- Genetic predisposition: Individuals with a family history of rosacea are more likely to develop the condition.
- Innate immune system dysfunction: An abnormal production of cathelicidin, a protein that fights bacteria but can also trigger inflammation and activate immune responses.
- Microorganism overgrowth: Inflammatory reactions can also be triggered by an increased presence of microorganisms normally found on the skin. Among them, the most studied is the Demodex folliculorum, a mite that lives in hair follicles.
- Ultraviolet (UV) radiation: Sun exposure can worsen rosacea by stimulating the release of vasoactive substances and free radicals, both of which promote inflammation.
- Excessive vasodilation: The release of various substances in response to different stimuli can lead to excessive blood vessel dilation.
Recommendations
What to avoid:
Managing rosacea requires avoiding triggers of facial flushing or flare-ups, such as:
- Sun exposure
- Intense physical activity
- Sudden temperature changes
- Psychological stress
- Alcohol consumption
- Spicy foods
- Harsh cosmetic products
- Creams or ointments with corticosteroids
Avoid using astringents, toners, and exfoliants, as they can irritate sensitive skin. Instead, opt for gentle cleansers and daily application of emollient creams specifically designed for rosacea-prone skin.
Importantly, corticosteroid creams should be avoided, as they may offer temporary relief but often cause rebound flare-ups when discontinued.
Can rosacea be treated naturally?
Rosacea is a chronic condition, so while it cannot be completely cured, several natural approaches can help reduce symptoms:
- Avoid direct heat sources on the face
- Minimize UV exposure
- Limit intake of hot or spicy foods and drinks
- Reduce or eliminate alcohol consumption
Daily use of broad-spectrum sunscreens is highly recommended.
Can I get rid of rosacea marks? Is there a specific cream?
There are several prescription topical treatments available, including:
- Azelaic acid
- Metronidazole
- Ivermectin
These have been shown to reduce inflammation and visible symptoms effectively. However, rosacea can resemble other skin conditions, so it’s essential to consult a dermatologist for an accurate diagnosis and appropriate treatment plan.
